Express Scripts, the pharmacy benefits management business of Evernorth, a subsidiary of The Cigna Group (NYSE: CI), today announced several actions to further evolve its pharmacy benefit management (PBM) model. The new solutions and capabilities will increase access to affordable medicines, and drive greater transparency and predictability. As part of its long-standing commitment to accelerate pharmacy care and lower the cost of prescription drugs for more than 100 million Americans, Express Scripts is further aligning incentives across the pharmaceutical supply chain, consumers, and clients, with new products available starting in summer 2023.
Driving Down Costs for Consumers
Express Scripts is introducing a new and innovative solution, the Copay Assurance plan, which caps consumer out-of-pocket costs for prescription drugs under a client’s prescription drug benefit. This means customers enrolled in the program will pay no more than $5 for generics and specialty generics, $25 for preferred brand drugs, and $45 for preferred specialty brand drugs every time they fill a prescription. The program will immediately guarantee these lower out-of-pocket rates – customers will not have to wait to meet any deductible levels.
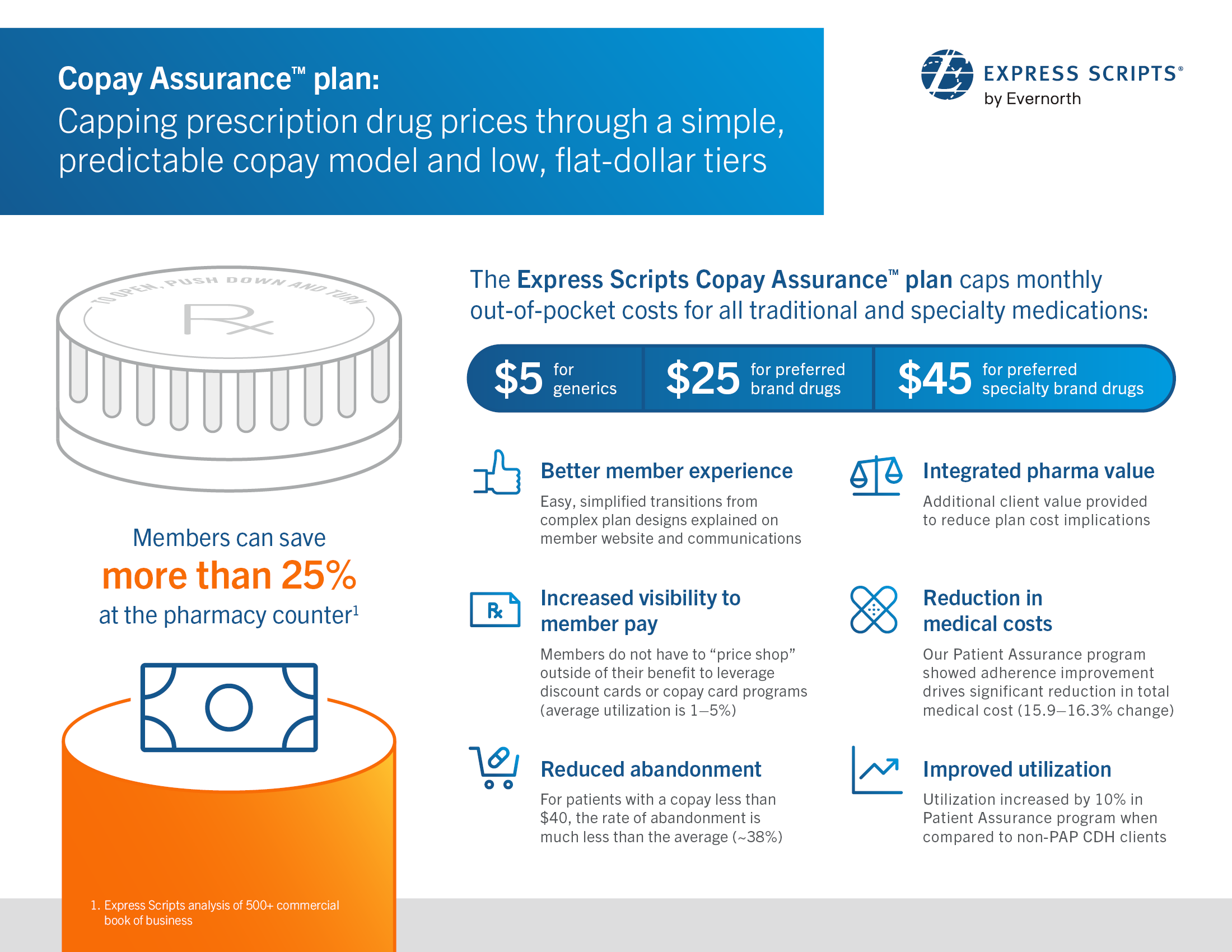
Express Scripts’ new Copay Assurance™ plan ensures consumers pay less out-of-pocket by capping copays on prescription drugs at $5 for generics, $25 for preferred brand drugs, and $45 for preferred specialty brand drugs.
“A prescription drug doesn’t work if it’s priced out of reach. Reducing out-of-pocket costs for consumers is the single best thing we can do to improve the health of those we serve,” said Adam Kautzner, Pharm.D., President of Express Scripts. “Express Scripts was first to deliver a $25 price cap on out-of-pocket costs for insulin and other diabetic treatments, which has saved consumers more than $45 million in two years. Our new Copay Assurance plan builds on this success and aggressively expands our efforts across medications to treat all diseases – providing millions more people with predictability and peace of mind at the pharmacy counter.”
Additionally, Express Scripts is working with employer and health plan clients to offer consultative options to bring better affordability and predictability. This includes: adopting the broadest lists of preventive prescription drugs that are either fully covered or covered at a discount, lower premiums and deductibles, and increased Health Savings Account contributions for lower- income consumers based on IRS income requirements.
Offering Clients a New Level of Transparency
Express Scripts’ new ClearCareRx offers employer, health plan, and government employer clients the option of a transparent economic model by providing clear and predictable costs for prescription drug benefits:
- Clients pay exactly what Express Scripts pays pharmacies for a prescription.
- Clients receive 100% of drug rebates that Express Scripts obtains by negotiating with pharmaceutical companies.
- Clients pay one simple fee to cover the administration of pharmacy benefits, PBM product services, reporting and analytics, and is 100% auditable.
- Provides guarantees that keep Express Scripts accountable to clinical and financial performance measures, including improvements in drug performance, adherence, and overall patient outcomes.

Express Scripts’ new ClearCareRx offers employer, health plan, and government employer clients the option of a transparent economic model by providing clear and predictable costs for prescription drug benefits.
“Expanding on our proven track record of driving transparency, ClearCareRx drives greater simplicity, with strategies to further reduce costs and improve health and pharmacy care. If we don’t deliver on a client’s goals, they pay less, guaranteed,” Kautzner added. “We are built to work on our clients’ terms. That means constantly coming to the table with innovative pharmacy benefits and tailored approaches that do more for them and the unique needs of their people.”
Enhanced Disclosures and Clarity
Express Scripts is further evolving its transparency to consumers and clients, and enhancing its disclosure practices, including:
- Demonstrating the value consumers and clients can expect from their pharmacy benefit services: Starting in 2024, prescriptions will include an easy-to-understand digital pharmacy benefits statement for consumers – sharing drug price information, out-of-pocket costs, and the value delivered by Express Scripts. This benefit will be implemented across all 65,000 pharmacies in Express Scripts’ networks, including Accredo® specialty pharmacy, and Express Scripts Pharmacy.
- Enhanced financial and fee disclosure for clients utilizing spread pricing: Express Scripts offers different PBM pricing options that clients can select based on their unique needs. Some of these options include spread pricing, a value sharing arrangement for the discounts Express Scripts negotiates with retail pharmacies for prescription medications.. Beginning with the 2023 plan year, Express Scripts will provide clients enhanced financial and fee disclosure regarding their spread pricing arrangements for Form 5500 reporting and other plan administration functions. The Form 5500 Series is a compliance, research, and disclosure tool for the U.S. Department of Labor (DOL), other Federal agencies, Congress, as well as for plan participants and beneficiaries, and the private sector to assess employee benefit, tax, and economic trends and policies. Express Scripts will provide the same level of increased disclosure to its non-ERISA clients to help support them in understanding the services Express Scripts provides.
- Launch of a microsite providing disclosures, and filings with the SEC: Concurrent with the release of first quarter earnings by The Cigna Group, Express Scripts will launch a new microsite that will provide additional information about the Express Scripts model. The Cigna Group will also provide additional disclosures regarding its PBM business in its upcoming SEC 10-Q filing.
“Our mission is simple: lower the cost of prescription drugs for the one in three Americans we serve. Today’s actions demonstrate our ongoing commitment to that mission, and helps clients and consumers see the value of their pharmacy benefits at work more quickly in their daily lives. Because at the end of every prescription is a consumer and client putting their trust in us – that’s a responsibility that drives us each day,” Kautzner said.
As a leader in innovative solutions designed to drive meaningful consumer and client outcomes and performance, the initiatives announced today represent Express Scripts’ long-standing commitment to advance the PBM model. Previous programs include SafeGuardRx®, Embarc Benefit Protection®, and the Patient Assurance Programsm – which combined with effective negotiation and medical management, saved consumers and clients more than $56 billion in 2022.
About Evernorth Health Services
Evernorth Health Services creates pharmacy, care and benefits solutions to improve health and increase vitality. We relentlessly innovate to make the prediction, prevention and treatment of illness and disease more accessible to millions of people. Evernorth capabilities are powered by our businesses, including Express Scripts, Express Scripts® Pharmacy, Accredo, eviCore and MDLIVE, along with holistic Evernorth platforms and solutions that move people and organizations forward. All Evernorth solutions are serviced and provided by or through operating affiliates of Evernorth Health, a wholly owned subsidiary of The Cigna Group (NYSE: CI), or third-party partners. Learn more at evernorth.comThis link will open in a new tab..
CAUTIONARY NOTE REGARDING FORWARD-LOOKING STATEMENTS
This press release, and oral statements made in connection with this release, may contain forward-looking statements within the meaning of the Private Securities Litigation Reform Act of 1995. Forward-looking statements are based on Cigna’s current expectations and projections about future trends, events and uncertainties. These statements are not historical facts. Forward-looking statements may include, among others, statements concerning future financial or operating performance, including our ability to (i) further evolve our pharmacy benefit management model, (ii) increase access to medicines, (iii) drive greater simplicity with strategies to further reduce cost and improve health and pharmacy care, (iv) drive transparency and predictability to consumers and clients, (v) enhance disclosure practices; and (vi) work with employer and health plan clients to increase affordability and predictability; the potential for our programs to increase health outcomes; future growth, business strategy and strategic or operational initiatives, including those related to the Copay Assurance plan, ClearCareRx and our enhanced disclosure initiatives; and other statements regarding Cigna’s future beliefs, expectations, plans, intentions, liquidity, cash flows, financial condition or performance. You may identify forward-looking statements by the use of words such as “believe,” “expect,” “project,” “plan,” “intend,” “anticipate,” “estimate,” “predict,” “potential,” “may,” “should,” “will” or other words or expressions of similar meaning, although not all forward-looking statements contain such terms.
Forward-looking statements are subject to risks and uncertainties, both known and unknown, that could cause actual results to differ materially from those expressed or implied in forward-looking statements. Such risks and uncertainties include, but are not limited to: our ability to achieve our strategic and operational initiatives; our ability to adapt to changes in an evolving and rapidly changing industry; our ability to compete effectively, differentiate our products and services from those of our competitors and maintain or increase market share; price competition, inflation and other pressures that could compress our margins or result in premiums that are insufficient to cover the cost of services delivered to our customers; the potential for actual claims to exceed our estimates related to expected medical claims; our ability to develop and maintain satisfactory relationships with physicians, hospitals, other health service providers and with producers and consultants; our ability to maintain relationships with one or more key pharmaceutical manufacturers or if payments made or discounts provided decline; changes in the pharmacy provider marketplace or pharmacy networks; changes in drug pricing or industry pricing benchmarks; political, legal, operational, regulatory, economic and other risks that could affect our multinational operations, including currency exchange rates; the scale, scope and duration of the COVID-19 pandemic and its potential impact on our business, operating results, cash flows or financial condition; risks related to strategic transactions and realization of the expected benefits of such transactions, as well as integration or separation difficulties or underperformance relative to expectations; dependence on success of relationships with third parties; risk of significant disruption within our operations or among key suppliers or third parties; our ability to invest in and properly maintain our information technology and other business systems; our ability to prevent or contain effects of a potential cyberattack or other privacy or data security incident; potential liability in connection with managing medical practices and operating pharmacies, onsite clinics and other types of medical facilities; the substantial level of government regulation over our business and the potential effects of new laws or regulations or changes in existing laws or regulations; uncertainties surrounding participation in government-sponsored programs such as Medicare; the outcome of litigation, regulatory audits and investigations; compliance with applicable privacy, security and data laws, regulations and standards; potential failure of our prevention, detection and control systems; unfavorable economic and market conditions including bank failures, the risk of a recession or other economic downturn and resulting impact on employment metrics, stock market or changes in interest rates and risks related to a downgrade in financial strength ratings of our insurance subsidiaries; the impact of our significant indebtedness and the potential for further indebtedness in the future; risk related to our reinsurers; as well as more specific risks and uncertainties discussed in our most recent report on Form 10-K and subsequent reports on Forms 10-Q and 8-K available through the Investor Relations section of www.cigna.com. You should not place undue reliance on forward-looking statements, which speak only as of the date they are made, are not guarantees of future performance or results, and are subject to risks, uncertainties and assumptions that are difficult to predict or quantify. Cigna undertakes no obligation to update or revise any forward-looking statement, whether as a result of new information, future events or otherwise, except as may be required by law.